

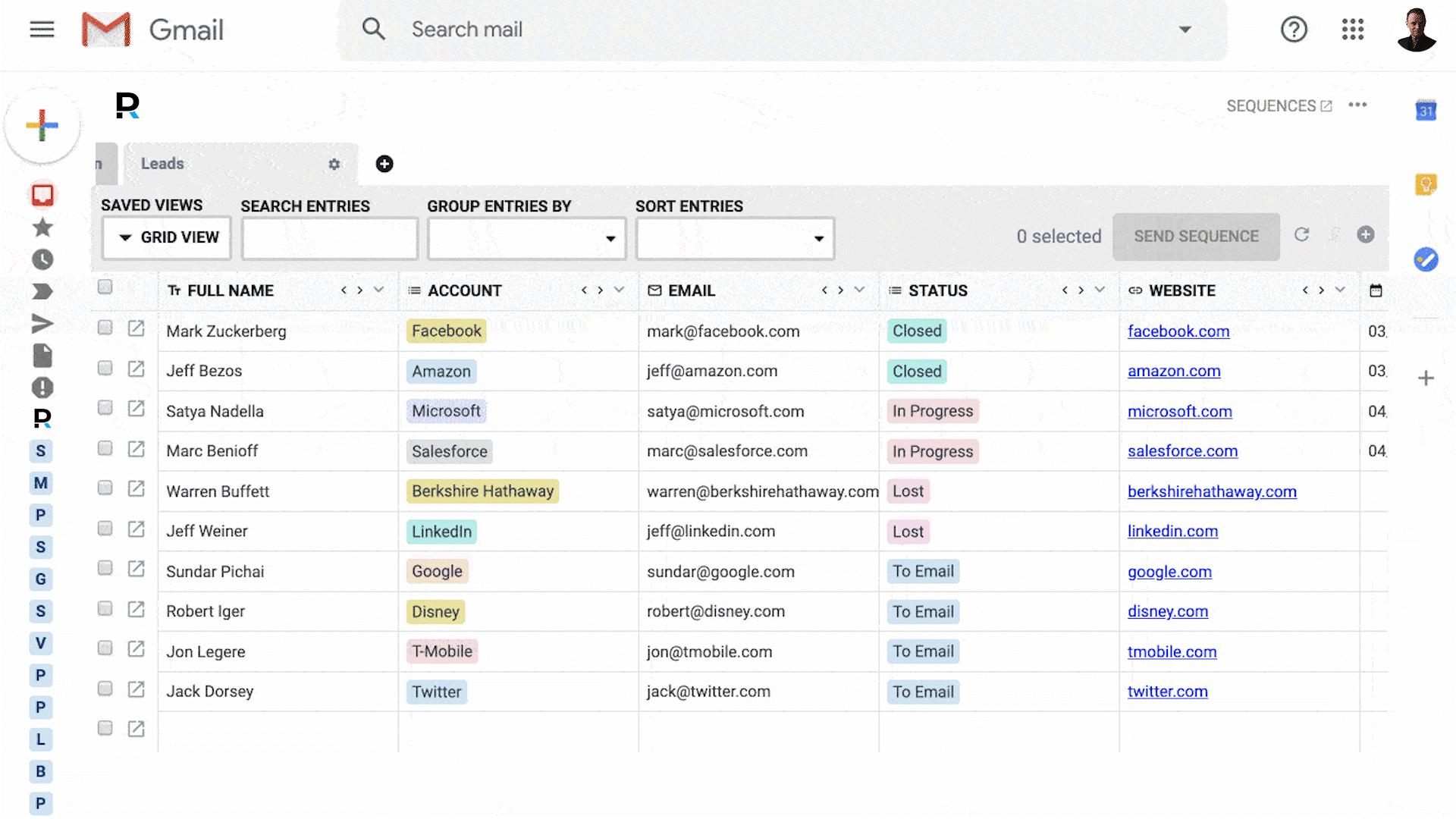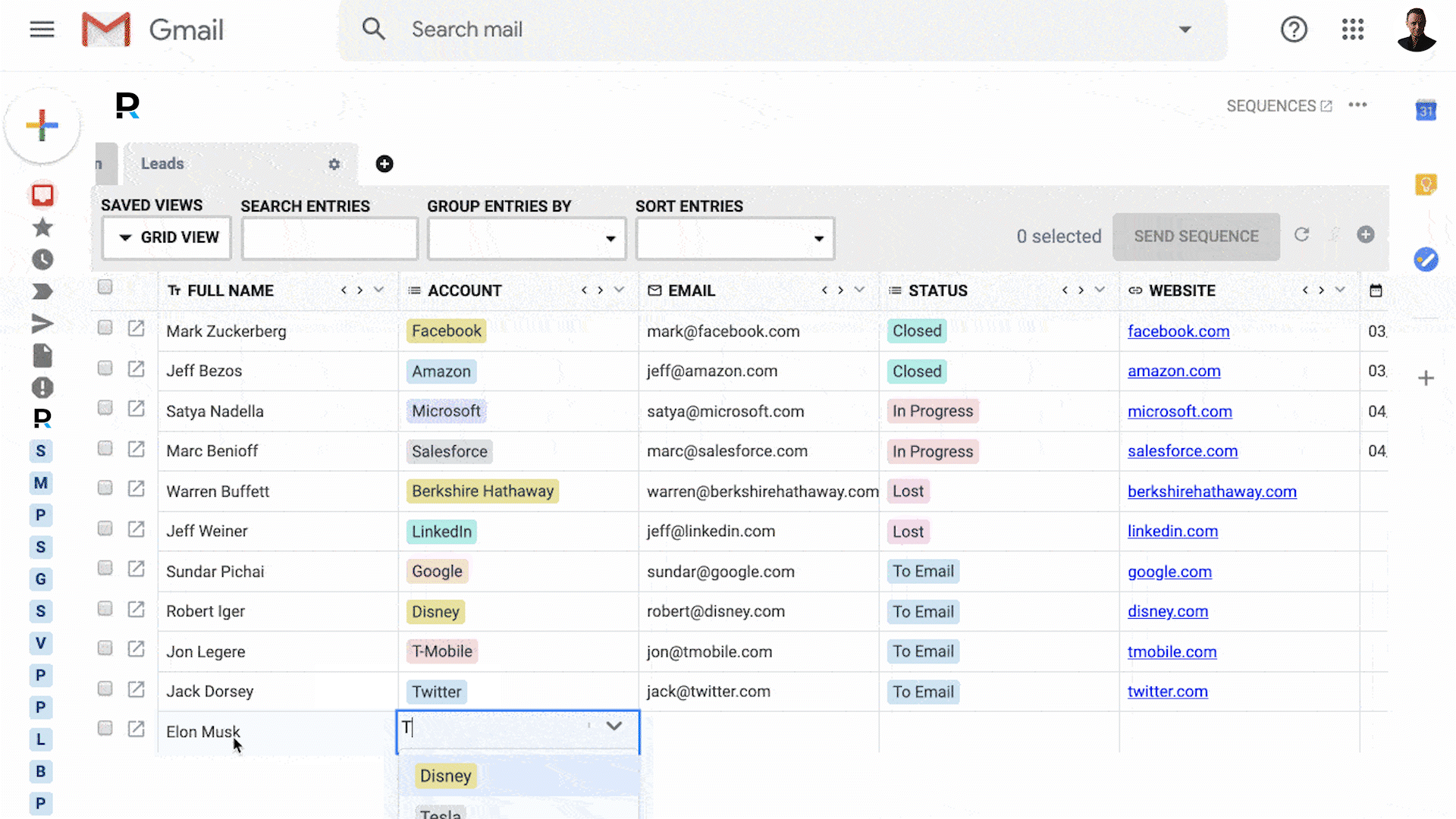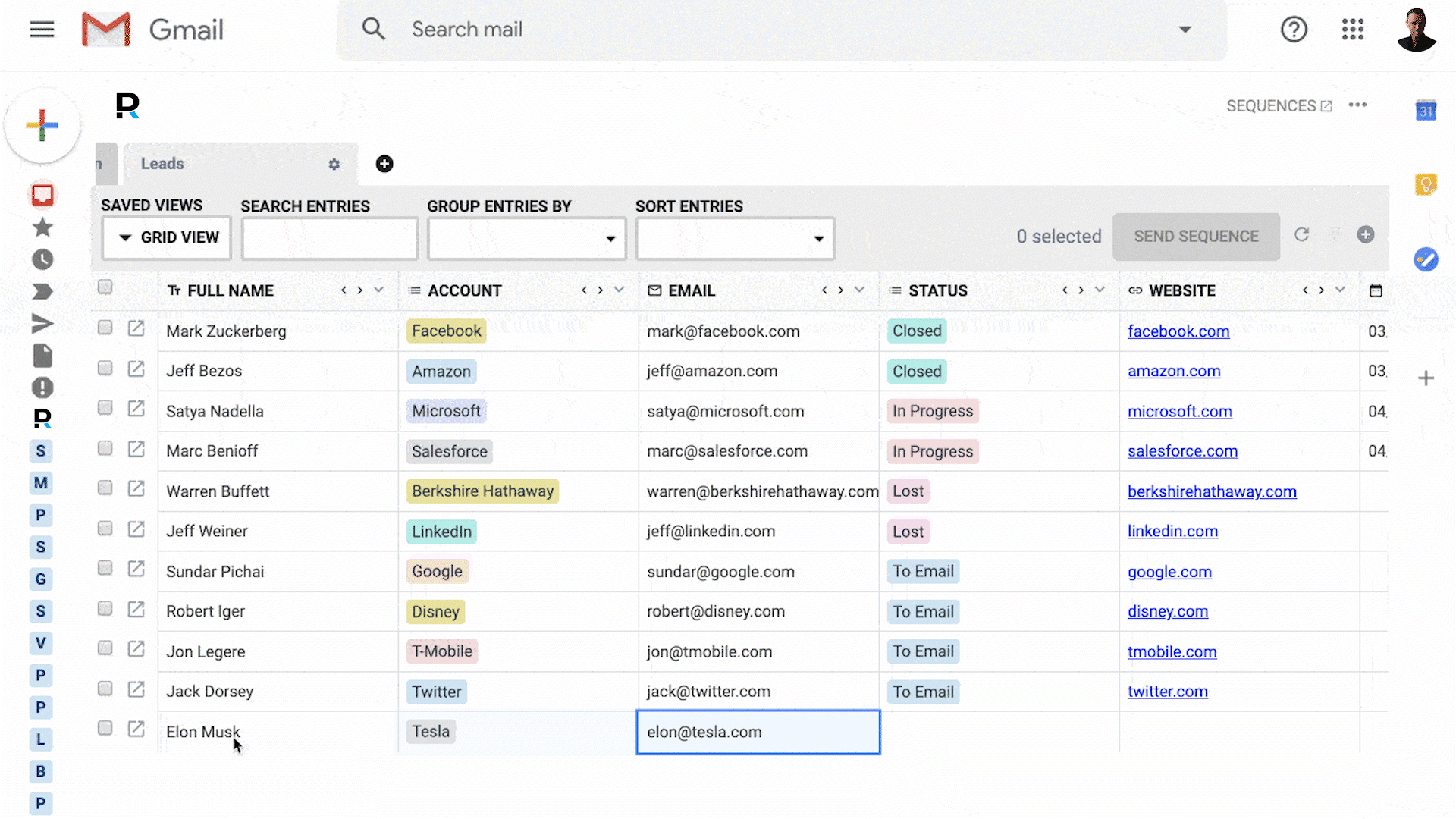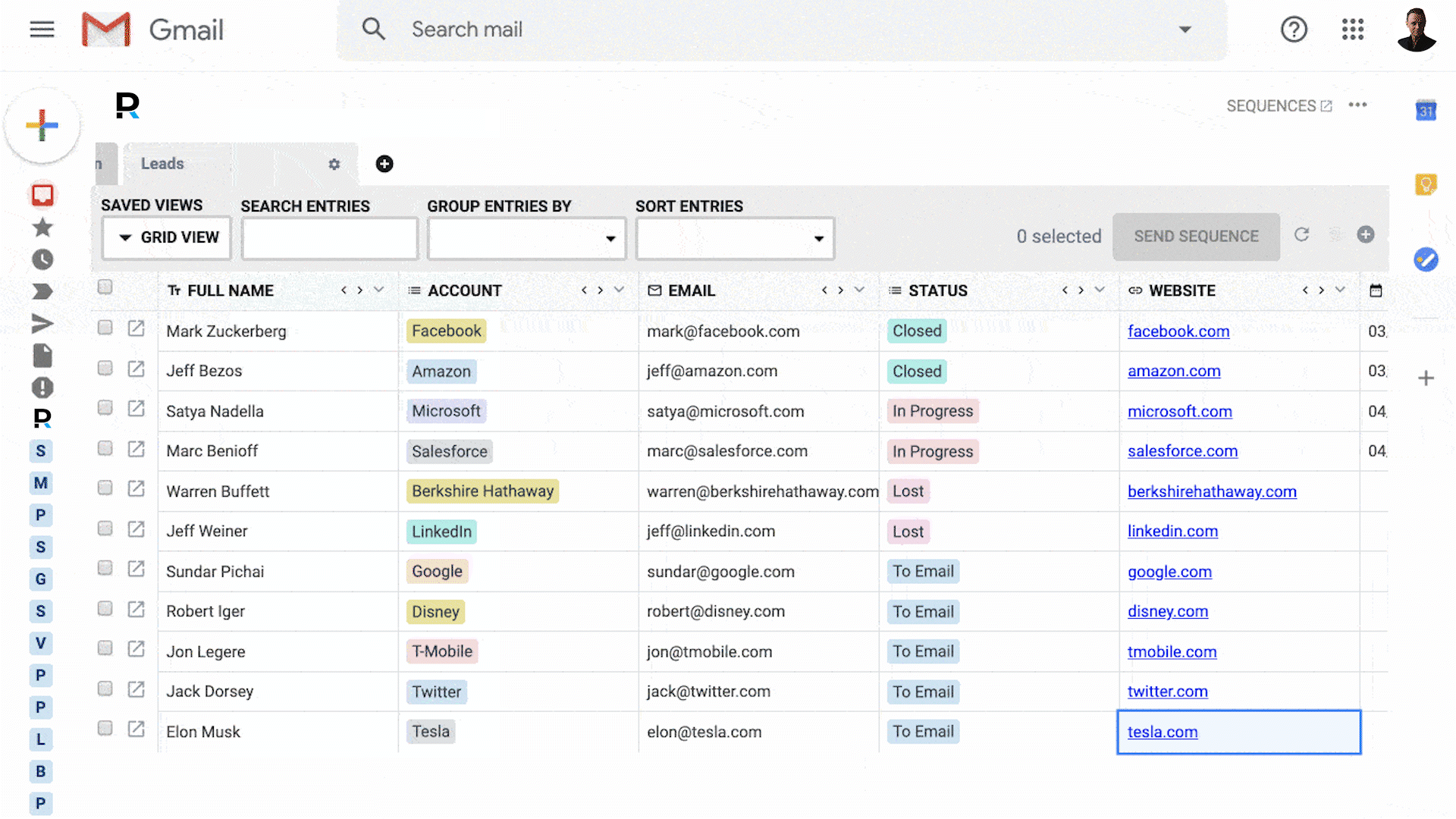

Your business runs on email - so why are you using tools that don't integrate with it?
Powerful CRM inside Gmail
Install with one click
100% integrated with Gmail & G Suite

Get replies, close deals, and attract customers. All inside Gmail.
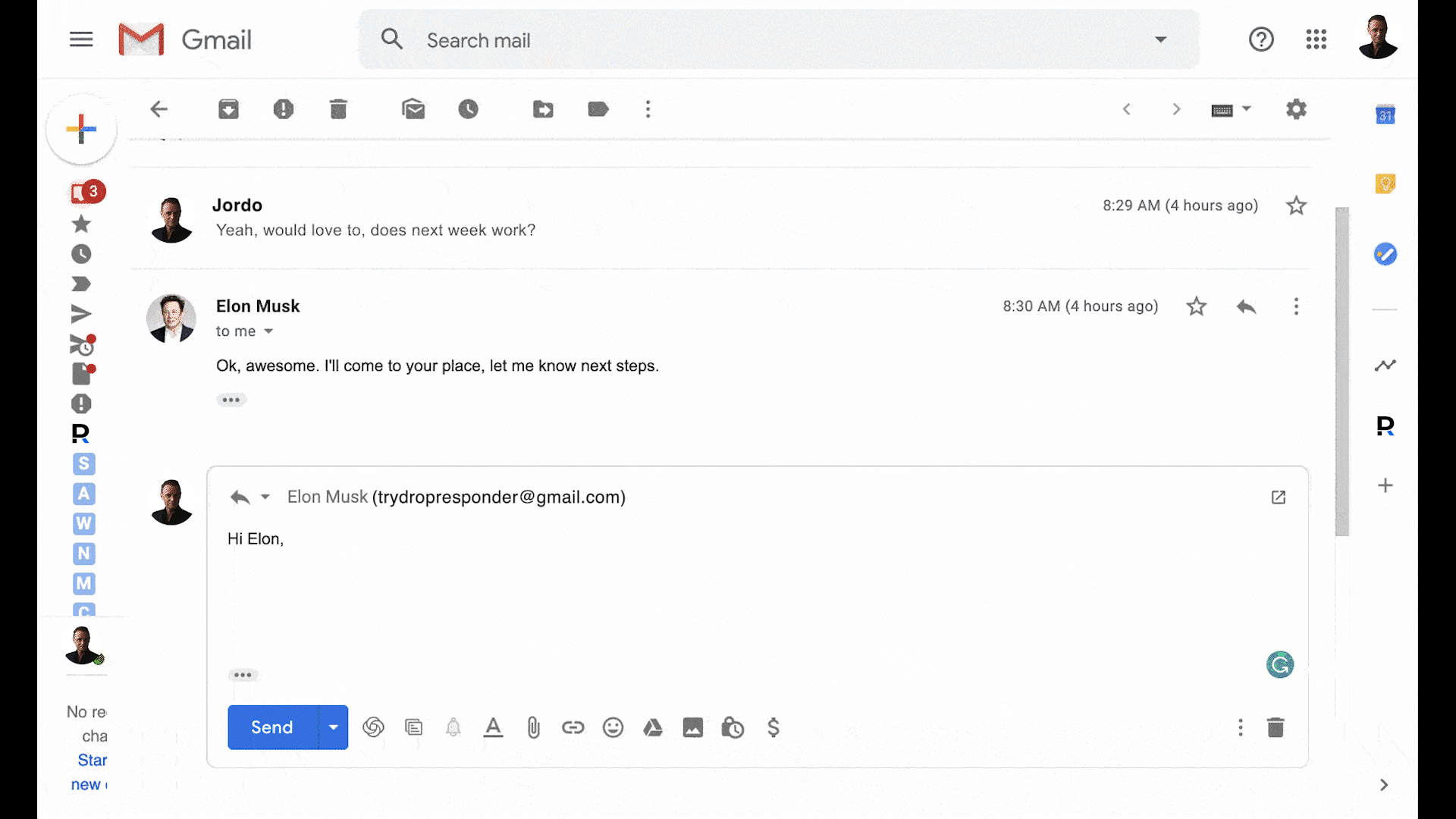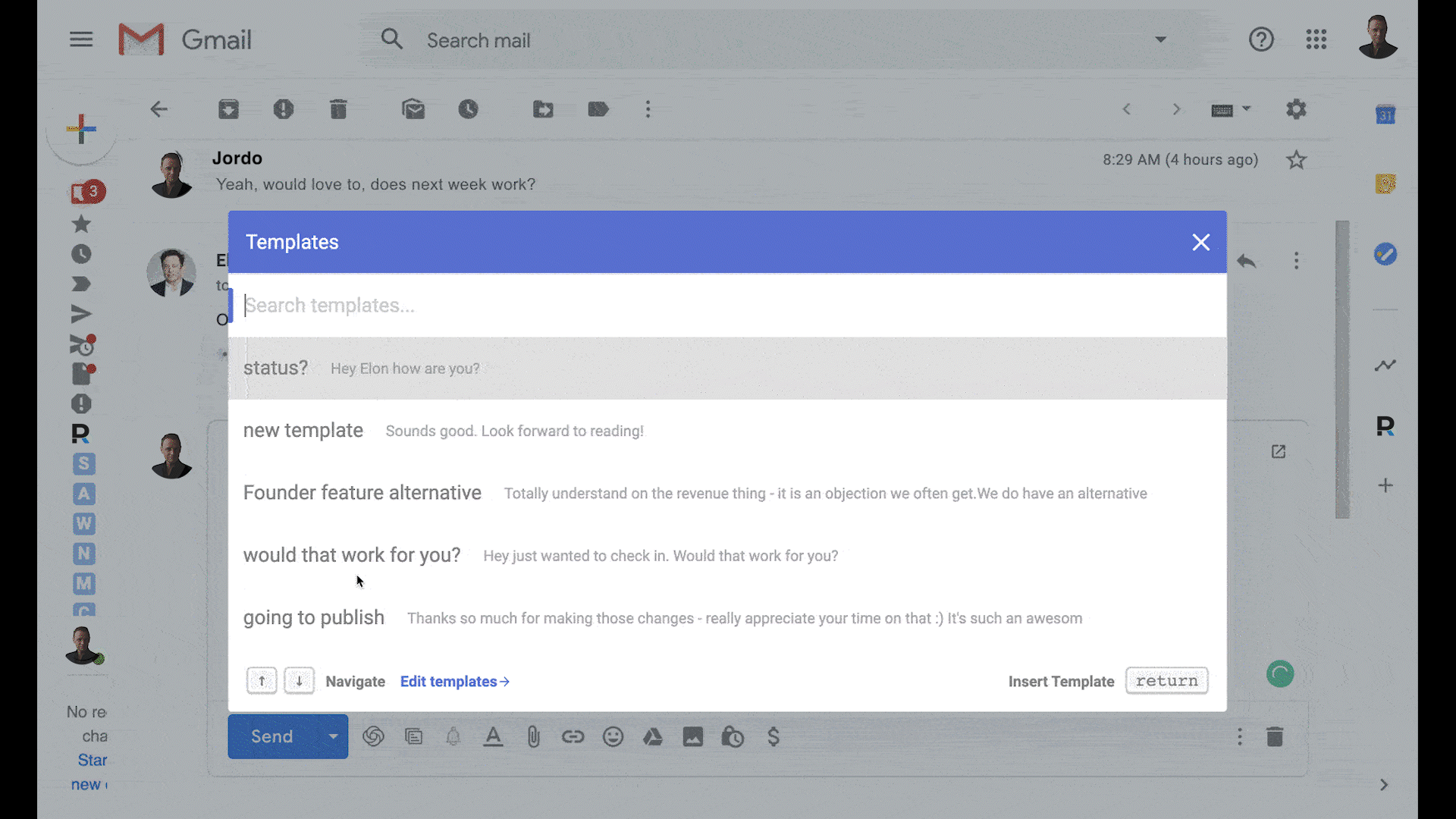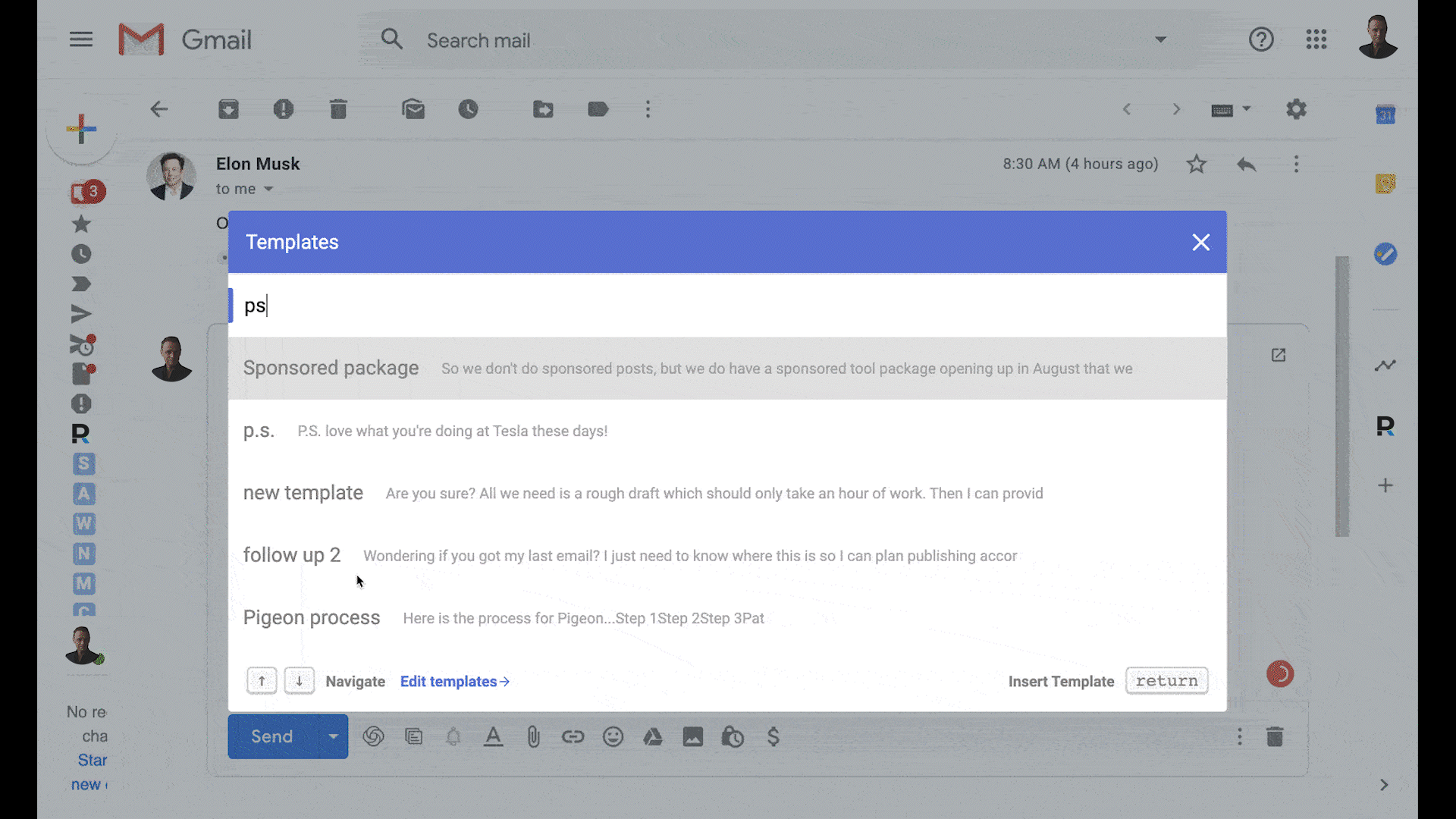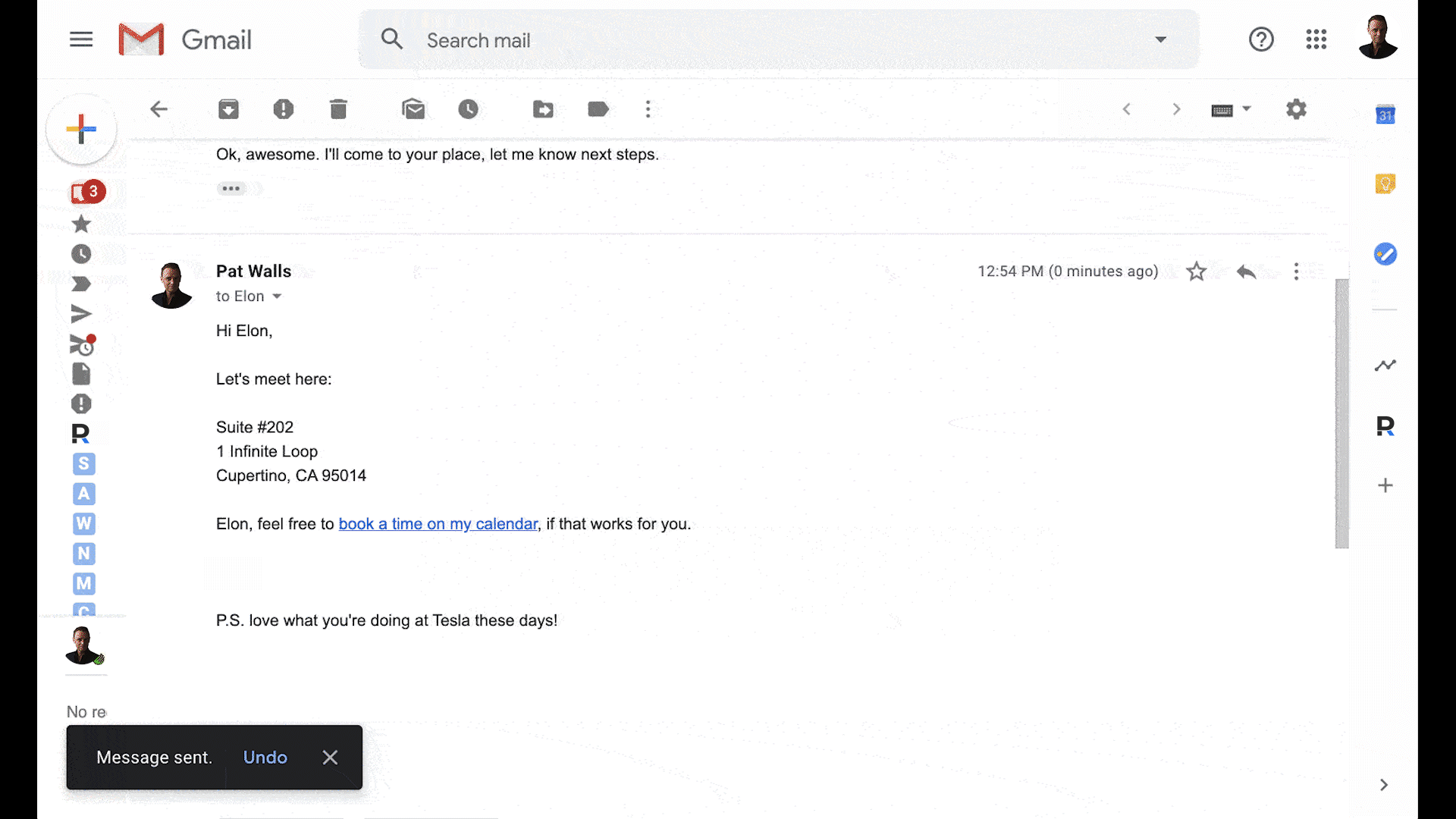
Send sales campaigns inside Gmail
Get more replies with automated follow ups
Revive lost customers with sequences

Crush your inbox with our productivity tools.
Process email 2x faster with keyboard shortcuts
Know when your emails are viewed and clicked
Integrate with 1000's of apps with Zapier















